Originally published in Volume 37 Issue 4 of Artificial Organs, 05 April 2013

The first hemodialysis was done by Pim Kolff on March 15, 1943 in the hospital in Kampen, Holland, and I believe the first in the USA was done at the Peter Bent Brigham Hospital in Boston, MA, in 1946 or 1947 by John Merrill and George Thorn. It was late academic year 1949 or the beginning of 1950 that I became John Merrill’s designated helper. It began with shaking hands in the lobby of the Peter Bent Brigham Hospital and immediately going to the lab to measure serum and urine osmolalities by freezing point depression before I even put my suitcase down. After finding a room, I went to the dialysis unit to boil cellophane and then help roll it on the drums of the kidney. John was my teacher but the next person I met, William Murphy (Bill), was my tutor. Bill had the heart of a clinician but the mind of an engineer who thought with his fingers and made sure I understood how to manage the artificial kidney under all circumstances. Then, I practiced heating Tygon—drawing it out to make cannulae of different sizes which provided vascular access to connect the patient and artificial kidney. Finally, a surgeon was needed and Charlie Hufnagel, yet to become famous, filled that role at the Brigham and then at Georgetown where for over 6 h of work he sometimes received US$25.00.
The patients transferred to the Brigham were posttraumatic—be it injuries, fractures, crushes, surgical complications, gynecological and obstetrical emergencies, transfusion reactions, poisonings, even plain water irrigations. They had received intensive care and were stabilized but there was little or no urine output with continuing tissue breakdown. Cellular components and elements accumulated in the blood due to lack of kidney function—this complication nearly doubles the mortality rate. The stakes were high as the body had been damaged, but the kidneys had only been stunned and within 30 days could recover if given the chance.
The medical care was personal. One or two doctors directed everything—the times and frequency of dialysis, the participation of the specialists, and the daily management of the patient for as long as it took. We were internal medicine clinicians, whole body doctors, wearing stethoscopes, using blood pressure cuffs, carrying reflex hammers: John had a urinometer in his pocket, I had an otoscope and eyepiece in mine. He was in his second year without a vacation, I did not want one and was thrilled to be saving lives rather than being limited to prescribing phenobarbital, digitalis, a mercurial diuretic, and cautious amounts of penicillin. We were pleased if our efforts were successful, sad if the patient died in the first 7–10 days, bitter if on day 21.
I returned to Georgetown with the artificial kidney and a confidence provided by John finally taking time off, allowing me to be in charge long enough to run a patient and gain the Brigham embrace (Fig. 1). Georgetown was the first satellite, had John’s continuous support and in the next 18 months confirmed its worth: life saving in a woman with mercury poisoning who was highly catabolic with rectal hemorrhaging; life extending in the case of a man with terminal renal failure which enabled him to return to Florida and sign papers; application to acetylsalicylic acid intoxication 1, the same drug shown to be hemodialyzable by Abel et al. in 1913–1914 with the original artificial kidney and suggesting such use. Drug removal also funded the “kidney” at Georgetown. This case was memorable if not historic because the Kolff–Brigham version was demonstrated for Leonard Rowntree whose job on the original kidney was to actually operate the apparatus after crushing leeches to obtain the anticoagulant. He also learned of the careful work underway on barbiturates 2. He told us the artificial kidney might have come to an early and final end had he not caught it after letting it slip from his grip on a bus in Brussels.

Figure 1
My next 18 months were spent on board USS Macon CA 132, command ship 6th fleet. It is notable that at the tea for new crew members, I challenged Admiral W.S. Parsons on the physical half-life of tritium which resulted in his interest in my work on total body fat, rearranging my algebra, and even reading The Treatment of Acute Renal Failure in the Armed Forces Medical Journal. I, in turn, learned Oppenheimer had visited him 2 weeks before I came aboard and that he insisted on being on board the Enola Gay to make sure that if the maximally burdened plane failed to take off, the bomb would not go off. If it had, little would have been left of Tinian Airfield and I would never have met John Merrill who was a medical officer serving there. Beyond that, other notable happenings onboard included failing to make helmsman, being rescued by an airlifted real surgeon on a deeply buried retro cecal appendix, doing sick call, being the authority on urethritis, being the boxing coach, and putting on fights in France, Italy, and Spain. In a long, severe gale in the North Atlantic the main deck was cracked. Shortly afterwards, I received orders to report to the US Naval Hospital (USNH) Oakland. I remain proud to have been aboard the USS Macon.
At the USNH Oakland, I was assigned to the medical service with additional duty of setting up and operating a Brigham-like unit at the Metabolic Research Unit. It was, in 1953, the first on the West Coast (Fig. 2). The Army team was already engaged in studies of acute renal failure in Korea. There was no formal relationship, simply one of same purpose, saving lives, bilateral pride, and lifelong friendships. The Army researchers encouraged our development of peritoneal lavage (dialysis) as a needed addition in the management of acute renal failure. At the time there was one artificial kidney in Korea and one on the West Coast. The studies done by the Army were the finest ever done on battle casualties and this, I suspect, includes the subsequent engagements. The work done at USNH Oakland was confirmatory in terms of the value of hemodialysis but there were broader contributions of major importance such as the early detection, progress, and severity of renal excretory failure that could be followed with measurements of serum and urine creatinine. Peritoneal dialysis quickly became a treatment, thanks in part to Bill Murphy’s catheter and the first focused and detailed studies in 10 patients with Goodpasture’s syndrome which contributed new concepts to the pathogenesis of renal disease. Others could be listed.
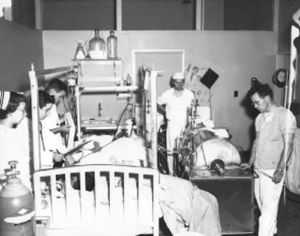
Figure 2
Barbara Coleman, Frances Pac, and Leona Jackson were a few of the nurses responsible for all the support material and supplies and the readiness of the unit at the Brigham, Georgetown, and USNH Oakland. They were largely responsible for the early success, but I think it was also due to what they stand for—help and hope—and when they were there I felt I was on the right side!
By the end of the 1950s, the artificial kidney, kidney transplantation, and peritoneal dialysis had settled in and even bigger challenges arose. Medical ethics had vaulted from Hippocrates to Belding Scribner. The problems of real-life extended care and funding were faced by a group of dedicated doctors, the Medical Society, and a raft of wonderful citizens of Seattle with the university lending assistance. The forefront shifted from the East to the West Coast.
Biosketch
Dr. Doolan was born in 1924 and received his undergraduate education at Georgetown and Duke Universities and completed his graduate and postgraduate studies at Georgetown, Boston City Hospital, and the Peter Bent Brigham Hospital. He joined the US Navy in 1942 and served aboard the USS Macon and at the US Naval Hospital Oakland. He conducted research at the Brookhaven National Lab and the Naval Medical Research Institute prior to continuing his work at the Medical College of Virginia as an associate dean and at St. Mary’s Hospital in Connecticut where he assisted in the development of the Regional Medical Program and served on the commission establishing the End-Stage Renal Disease program in Connecticut. He was clinical Professor of Medicine at Yale. During his distinguished naval career and afterwards, Dr. Doolan established the second hemodialysis center in the USA and also advanced the use of peritoneal dialysis. His early work and subsequent research helped define the field of nephrology as a specialty. He has worked in all aspects of medicine from clinical treatment, to establishing research centers, to teaching, to bench research. He also participated in study sections and review committees for the federal government and is involved in policy and politics. He has received many awards and accolades for his achievements including the T. Stewart Hamilton, MD Distinguished Service Award in 1998 for his tireless efforts toward the advancement of health care, presented to him at the 80th Annual Meeting of the Connecticut Hospital Association. Dr. Doolan has four children and eight grandchildren and lives in Phippsburg, ME with his wife Mary Ellen, where he continues to study many aspects of the human condition.

